For A Veteran Telemedicine Doctor, Pandemic Confirms Need to Improve Systems of Care
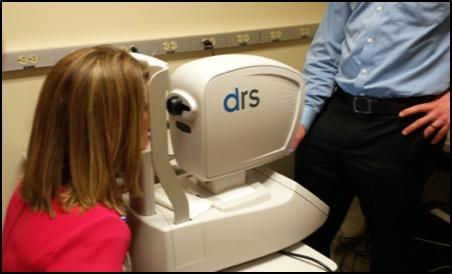
LEXINGTON, Ky. (Aug. 20, 2020) – By the time the pandemic forced many patients and providers into telemedicine, ophthalmologist Ana Bastos de Carvalho had been using it for years. As co-founder of UK’s Global Ophthalmology (UKGO) program, she has helped build and expand a statewide telemedicine eye screening program for diabetic patients in disadvantaged rural and urban communities.
Diabetes damages the eyes by causing blood vessels to become either leaky or thick and overgrown, so all patients need eye screenings every year. But many Kentuckians with diabetes don’t have insurance or live near an eye clinic, which means they don’t get necessary preventive care to protect their sight. Screening rates in many Kentucky communities are as low as five percent, according to Bastos de Carvalho.
“I’m originally from Portugal where we have universal health care. When I came to the US and was confronted with the health care system here, I wasn’t comfortable practicing medicine without doing something to serve people who don’t have proper access to care because they’re uninsured or far from services. I couldn’t sleep at night thinking I would only be serving people who had good access to care, while many people who needed care couldn’t get it,” she said.
Bastos de Carvalho and UKGO co-founder Dr. Eric Higgins have worked to close the gap in care by partnering with 39 mostly primary care clinics across Kentucky to provide eye screenings via telemedicine. Over the past seven years, Bastos de Carvalho, Higgins, Rob Sprang (UK Telecare’s Director), and Dr. Kim Northrip and Jasleen Chahal from UK’s CE Central have secured multiple grants that provided cameras to the clinics, which then send images of patients’ eyes to UK to be interpreted. Since beginning the program in 2014, screening rates among patients of participating clinics have doubled, on average.
“Dr. Higgins and I screen around 400 patients per month”, Bastos de Carvalho said.
“Diabetes patients need to have an eye screening every year, even without symptoms, so that we can diagnose and treat the disease in a timely manner. With telemedicine, the patient doesn’t have to take half a day to get to an eye specialist (who could be very far from them) and have their eyes dilated for an exam.”
Between 15 and 20 percent of patients seen through UKGO have some sort of referable pathology, whether diabetic retinopathy or other diseases like macular degeneration or glaucoma, and need to see a specialist for treatment.
To make the UKGO telemedicine network as effective as possible, Bastos de Carvalho is using implementation science to study why some clinics underutilize their cameras and thus miss opportunities for eye screenings. With the support of UK’s Physician Scientist Training program and mentorship from researchers with expertise in implementation science, she designed a study to methodically identify what prevents and what supports the use of eye screening cameras by clinic health care professionals.
“We found several different reasons for underutilization of the cameras—factors related to clinic workflow, relative priorities of the clinic, shortage of staff and time, technical issues with the equipment, staff learning how to use the cameras and feeling capable of taking appropriate images,” she said.
After she and Higgins validate their findings about barriers and facilitators of camera use, they will design and offer implementation packages to the sites to help them improve screening rates.
“The mentorship I received in implementation science from Dr. Tina Studts and Dr. Jamie Studts (who have since left UK) was invaluable. I couldn’t have done this research without it,” Bastos de Carvalho said. “And I wouldn’t be able to do this work if I didn’t have the support of the Physician Scientist Training program, or the backbone of the screening network initiated by Eric Higgins and Rob Sprang”.
Now in the midst of a pandemic, Bastos de Carvalho’s clinical work has remained at full speed and her research on improving the use of telemedicine has taken on new urgency.
“Our research work is now even more important than before, as we strive to improve access to diabetic eye screening via telemedicine, a service that has become of paramount importance with COVID-19.”
Bastos de Carvalho’s dedication to providing care for underserved communities is deeply rooted. Her father was an ophthalmologist, and the family lived in several developing countries while growing up.
“I witnessed a lot of poverty and inequality in healthcare, and I’ve always felt I needed to do something for people who can’t access care.”
She came to UK as a post-doctoral scholar seven years ago to do basic science research in ophthalmology. When she was invited to stay in the department as a clinician-scientist, she agreed on the condition that she could change her focus from basic science to working with underserved populations. She received overwhelming support and advocacy from her department chair, Dr. Andrew Pearson, and start-up funding from the College of Medicine Dean’s Office to support a post-doctoral scholar and a research assistant for her work.
In addition to the telemedicine program, UKGO operates outreach clinics in Kentucky (on pause due to the pandemic), has developed partnerships in Haiti and Ecuador to help train ophthalmologists in those countries, and plans to launch a Global Ophthalmology Fellowship at UK in 2021. Through UK GO, the UK Department of Ophthalmology is also the first ophthalmology program in the country to offer an official global health track during residency, and has just admitted the first residents into this track. The two selected residents are working on clinical and research projects to increase equity in eye health in Kentucky and abroad.
“All faculty and staff at the Department of Ophthalmology are an integral part of the success of UK GO, and the unconditional support we have from our chair, the CCTS, and the Dean’s office, has been paramount. There’s really no better place or partners for me to do this work,” Carvalho said.
The Physician Scientist Training Program is funded by the UK College of Medicine Dean’s Office and facilitated by the UK Center for Clinical and Translational Science as part of the KL2 Career Development Training Program cohort, which is funded by a Clinical and Translational Science Award.
Media Contact: Mallory Profeta, mallory.profeta@uky.edu
